Over the past decade consumer-driven health plans (CDHPs) have caught on with employers as a way to reduce the costs of providing health care benefits—primarily by making employees responsible for a larger share of their medical expenditures.
CDHPs include health reimbursement arrangements (HRAs), employer-funded plans that give workers money to put toward insurance premiums and out-of-pocket medical expenses, and health savings accounts (HSAs), tax-exempt funds owned by employees that can be used to pay for health care. Both employers and workers can contribute pretax dollars to an HSA.
HSAs, and often HRAs, work in tandem with health insurance policies carrying high deductibles, either sponsored by the employer or purchased by the worker in the individual insurance market.
Since 2003, when Congress created HSAs, consumer-driven plans have grown from a niche product into a common approach to packaging health care benefits. In a survey by the Kaiser Family Foundation and the Health Research & Educational Trust, 15 percent of U.S. firms reported offering high-deductible savings plans last year, up from 4 percent in 2005. CDHPs were most popular with large employers with 1,000 or more workers; about one-third of firms with 1,000 or more workers sponsored such plans last year.
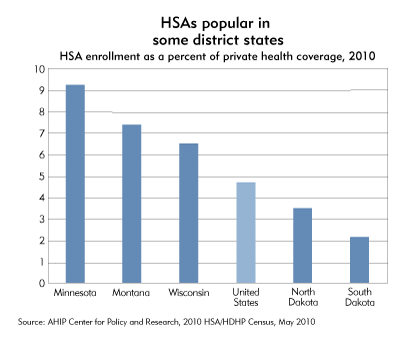
Another survey of HSA usage by America’s Health Insurance Plans, a national trade association for health insurers, found that 10 million people nationwide were covered by such plans last year, a 25 percent increase over 2009. Among district states, HSA enrollment was highest in Minnesota—about 361,000 workers and their dependents. In that state and in Wisconsin and Montana, HSAs accounted for a larger share of private health insurance coverage than in the country as a whole (see chart).
For employers, the attraction of CDHPs is obvious: lower insurance premiums. With both types of plan, an employee pays medical bills out of his or her account—or, if necessary, the employee’s own pocket—until the insurance deductible is met. For HSAs, that bar is set fairly high—the legal minimum for family coverage in 2010 was $2,400. Lower premiums help employers to maintain coverage for their workers, even if it’s only catastrophic coverage.
For workers and self-employed individuals, such plans are tax-advantaged savings vehicles; any unspent funds can be rolled over to the next year or banked for retirement.
CDHPs and high-deductible plans in general also hold out the promise of cutting overall insurance and health care costs. By giving consumers more control over health care expenditures, the plans encourage them to spend more judiciously, seeking treatment only when necessary and comparing prices for prescription drugs and other medical goods and services.
“A high-deductible plan allows you to have choice, yet at the same time fiscal austerity,” said Stephen Parente, a health finance expert at the University of Minnesota who himself has an HSA to pay family health expenses.
In principle, consumers facing a larger share of health care costs should help control costs and reduce insurance premiums. A number of studies have found that CDHP enrollees spend less on health care than people in health plans with lower deductibles. But research into the cost effectiveness of CDHPs has also raised questions about the long-term impact of such plans on overall health care spending.
A recent study by Parente and other University of Minnesota researchers looked at employee health spending by four large companies that switched to CDHPs from traditional health plans. The study found that while employees’ health care spending dropped, they used less preventive care than before.
Less preventive care can save money, because not every screening or procedure is medically necessary. But by giving workers an incentive to skip certain screenings for serious health conditions such as cancer and diabetes, some health experts believe that CDHPs may increase total health care costs—and insurance premiums—down the road.